Table of Contents
The United States leads the world in health care spending. One might think that the more spent on healthcare, the better health outcomes would be. Surprisingly, this is not the case, as the U.S. ranks last in life expectancy and has the highest rates of chronic disease, suicide, avoidable deaths, and preventable disease-related hospitalizations. The reasons for this disparity are complex. The most concerning is that although there are significant health needs, there are significant affordability barriers to accessing health care. Serious inequities due to affordability barriers exist because populations that experience financial insecurity also experience poorer health outcomes.
The Commonwealth Fund has identified two changes that could have the greatest impact: making affordable health care accessible and expanding primary care systems. To accomplish this in a way that could have the greatest impact on the most vulnerable populations, equity must be a guiding principle.
The difference between equity and equality in healthcare
According to the Centers for Disease Control and Prevention (CDC), “health equity is when everyone has the opportunity to be as healthy as possible.” The World Health Organization (WHO) defines health equity as “the absence of unfair and avoidable or remediable differences in health among population groups defined socially, economically, demographically, or geographically.” Equity differs considerably from equality. “Equality is about the equal distribution of shares (of health or health care) so that each individual receives the same amount.” The WHO says that aiming for equity means “striving for the highest possible standard of health for all people and giving special attention to the needs of those at greatest risk of poor health.”
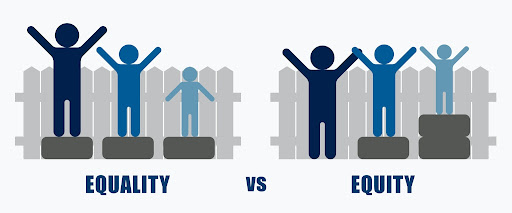
Therefore, expanding equitable affordable health care — specifically primary care — means doing so in a way that both prioritizes access for populations that have the most need and allows for equality amongst populations who have similar needs. The social conditions that influence health outcomes are referred to as “social determinants of health,” and influence inequities in health status. In higher education, equal access is not enough. Institutions that focus on equity over equality will ultimately better serve the wellness needs of all students.
Health inequalities for college students
In the U.S., Black people have the lowest pretax income levels, spend the highest proportion of income on housing, and experience the highest rates of unemployment. Hispanic/Latino people have the second-lowest pretax income levels and are the largest population with less than a high school education level in the U.S. The percentage of college students who receive grants is highest for Black and American Indian/Alaskan Native students. It is well documented that the oppression, racism, discrimination, and bias experienced by Black and American Indian/Alaskan Native people in the U.S. has resulted in significant, poor long-term health outcomes. The rates of death due to heart disease, stroke, prostate, and breast cancers are higher and life expectancy for Black people is lower than other populations. In addition, American Indians/Alaskan Natives experience higher rates of death due to diabetes, unintentional injuries, suicide, and assault/homicide and have the lowest life expectancy rates in the U.S.
Consequently, those who need health care the most, often can’t afford it. Therefore, they do not obtain health care that can prevent, identify, and treat disease and health issues early to increase life expectancy. Equitable health care must be delivered in a way for low-income and other students who struggle to access care that reduces barriers related to cost, provides comprehensive services, and strives to be representative of the populations served.
Create equitable healthcare solutions for students
An equitable telehealth solution for higher education
TimelyCare’s equitable approach to telehealth includes:
1. Partnerships with colleges and universities that offer no-cost telehealth services to students
For students who live off-campus, they need care when their campus health and counseling services are unavailable. For the more than 20% of institutions that do not offer on-campus services, telehealth can provide access to primary care where there were previously unmet needs. By offering no-cost services that students can utilize virtually wherever, whenever they need it, TimelyCare ensures that the barriers to affordable, equitable access and care are eliminated.
2. Proprietary health and well-being assessments that help campuses identify gaps in health equity
TimelyCare understands that student health and well-being is influenced by a variety of factors. This is why TimelyCare’s well-being assessment tool focuses on collecting information on areas including flourishing, resilience, help-seeking, healthy masculinity, femininity, substance use, and sleep.
3. Health and well-being content delivered through varied modalities and messaging to address the needs of diverse populations
Based upon the relative risks of disease and poor academic performance, TimelyCare’s four-year health and well-being curriculum is evidence-based and focuses content on areas of high risk, including mental and emotional well-being, substance misuse, sleep, and healthy relationships.
4. Basic needs services coordination to ensure holistic student support
Some of the factors that influence student health and well-being go beyond coughs, colds, and stress. Many students experience a lack of basic needs, such as consistent and reliable food, housing, transportation, childcare, technology, and more. Students struggle financially to balance these basic needs with the costs associated with furthering their education. The support and services coordination that TimelyCare provides takes into consideration students’ basic needs, and has a robust system in place to match students with campus-based or local resources that can assist them in maintaining their health, well-being, and educational status. As students’ wellness needs become more complex, higher education institutions must adopt a public-health approach to promoting student well-being on campus.
5. Student-centric mental and medical health care from a diverse network of providers with a variety of specialties
The college student population is increasingly diverse, representing identities, ethnicities, and experiences that may differ from existing campus support staff. While colleges and universities recognize the need to embrace diversity and inclusion and increase the population of staff and faculty of diverse identities, obstacles still exist. Only 6% of physicians identify as Hispanic/Latino, even though 19% of the U.S. population is Hispanic/Latino. Studies show that Black patients have better results when they are treated by Black healthcare workers, and Hispanic/Latino people have greater trust in medical professionals of the same race/ethnicity. As such, TimelyCare takes a strategic approach to hiring providers that represent the diverse identities and needs of college students. And students seeking care through TimelyCare can select a provider based on their identity and specialty. TimelyCare values, respects, supports, and honors the unique identities and characteristics of each member of our community of employees, partners, campuses, and students.
6. Team-based care with education and support from highly qualified professionals
Physical and mental health care providers are trained to assess every patient they interact with as a whole person, identifying needs that go beyond the initial concern. Working as a care team, TimelyCare’s social workers, primary care providers, mental health counselors, psychiatrists, and health coaches connect when students need additional support and services. In addition to in-the-moment education and referral during the care visit, a post-visit follow-up with every student offers additional education, support, and services coordination to ensure their needs have been met, which enables them to be well and thrive.
The role of telehealth in providing equitable care for college students
TimelyCare’s commitment to providing a best-in-class, cost-effective, advanced preventive and primary care solution enables:
- Equitable access to care
- Health improvement for students
- Quality of care in visits
- Enhanced student performance
Part of TimelyCare’s primary care offerings includes primary prevention services for mental and emotional health, including immediate emotional support (TalkNow) 24/7, 365 days a year, and scheduled teletherapy in all 50 states. TalkNow provides access to masters-level mental health professionals who are there to support students in crisis, and with non-crisis-related emotional health concerns.
Ninety-one percent of students connect to a TalkNow provider and 95% connect to any provider across all services in less than fifteen minutes.* This service is available to students 24/7 via video or phone. Offered in tandem with longitudinal counseling (48% of all visits, 69% of all mental health visits), TalkNow has had notable use (21% of all visits, 31% of all mental health visits).
Telehealth can serve the total health and well-being of students to enable them to be their best physical and emotional selves. TimelyCare’s higher education telehealth solution can do this through its commitment to delivering equitable care in a way that reduces barriers and increases optimal student health, well-being, and performance during their student journey and beyond.
Contact TimelyCare to learn more about equity vs equality in higher education healthcare.
Content contributor: Kristen Buglione, Healthcare Literacy Lead, TimelyCare
*based on connection times between January 2021 and April 2021






